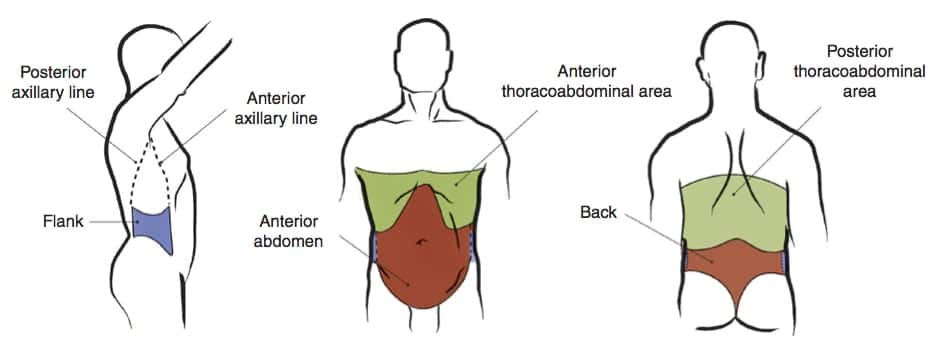
Blunt abdominal trauma (BAT) is a major medical emergency and accounts for up to 85% of trauma to the abdomen. Despite improved clinical practice, it remains to be a cause of substantial morbidity and mortality (Mehta et al., 2014).
Aetiology
It is known to arise majorly from Road traffic accidents, falls from a height, blows to the abdomen or assault, industrial accidents (Mehta et al., 2014; O’Rourke et al., 2020).
Clinical presentation
Patients usually present with abdominal pain. Other symptoms may include vomiting, dyspnoea, haematuria, and bleeding per rectum (Mehta et al., 2014; O’Rourke et al., 2020).
On examination, there may be signs of intraperitoneal injury including abdominal tenderness, distension (in the case of hemoperitoneum or pneumoperitoneum), ecchymoses such as grey Turner or Cullen sign, abdominal contusion as with lap belt sign, decreased bowel sounds, and blood per rectum following a digital rectal examination (Mehta et al., 2014; O’Rourke et al., 2020; Williams et al., 2013). If the patient has developed peritonitis, they could exhibit rigidity and rebound tenderness (O’Rourke et al., 2020). In the case of a haemodynamically unstable patient, signs of shock may ensue (cold clammy extremities, increased pulse rate, decreased blood pressure, increased respiration, altered mentation, and reduced urine output) (Williams et al., 2013).
Investigation
This depends largely on the haemodynamic state of the patient (Williams et al., 2013). Patients may be assessed initially by focused sonography for trauma (FAST) or a diagnostic peritoneal lavage (DPL). These are non-invasive tests that can be done bedside and simultaneously with resuscitation (Williams et al., 2013). FAST usually detects free intrabdominal fluid greater than 100 ml and can be used to determine risk stratification in stable patients (Dammers et al., 2017). Unstable patients with a positive FAST will require immediate intervention; FAST however may not be able to detect hollow viscus injury and has a high false positivity rate (Dammers et al., 2017; Williams et al., 2013). In DPL blood in the abdomen can be detected. It is more sensitive than CT and FAST for the detection of hollow viscus injuries (Jansen et al., 2008).
In stable patients, further assessment can be undertaken including CT scan, erect abdominal radiograph, diagnostic laparoscopy (Williams et al., 2013). A positive FAST in a stable patient will necessitate a confirmatory CT scan, which is useful in identifying solid organ damage and intraperitoneal haemorrhage (Dammers et al., 2017; Pande et al., 2017; Williams et al., 2013). An abdominal radiograph may suggest hollow organ damage by way of detection of free air under the diaphragm but cannot rule out intra-abdominal haemorrhage or solid organ injury (Jansen et al., 2008).
Management
All trauma patients should be initially assessed following ATLS protocols. This involves checking the patency of the airway and cervical spine stability, ensuring the patient is breathing, experiencing adequate circulation, has no further disability, and is exposed to identify any other hidden injury (O’Rourke et al., 2020; Raza et al., 2013).
A haemodynamically compromised patient should undergo immediate resuscitation (Williams et al., 2013). If the patient is not responding to resuscitation and has a positive FAST (free intraperitoneal fluid), emergency laparotomy is indicated (Jansen et al., 2008). Negative sonography however does not exclude injury and investigation of other sources of hypoperfusion is still indicated (Jansen et al., 2008). Other indications for emergency laparotomy include free intraperitoneal air, signs of peritonitis, and worsening clinical signs (O’Rourke et al., 2020).
In a stable patient, there is a need for observation and further investigation by CT to rule out organ damage and diaphragmatic injury (Mehta et al., 2014). The presence of solid organ injury may not require operative management (Jansen et al., 2008). If there is free fluid without organ damage then DPL may be performed to assess the nature of the fluid (Jansen et al., 2008). If the source of haemorrhage can be identified then therapeutic embolization may play a role in the control of bleeding (O’Rourke et al., 2020).
A normal CT may require observation and repeat history, physical and investigation (Jansen et al., 2008)